Introduction
As the warm weather approaches, many of us find solace in swimming pools, lakes, and oceans. While swimming is an excellent way to stay active and beat the heat, it also comes with certain health risks, especially concerning our ears. Swimmer’s ear, medically known as otitis externa, is a common and painful infection that affects the outer ear canal. In this article, we will explore the causes, prevention, and treatment of swimmer’s ear to ensure that you can enjoy your aquatic activities safely.
What is Swimmer’s Ear?
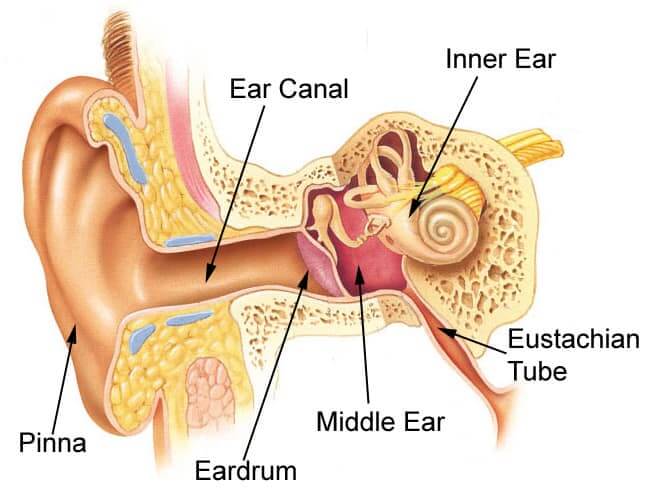
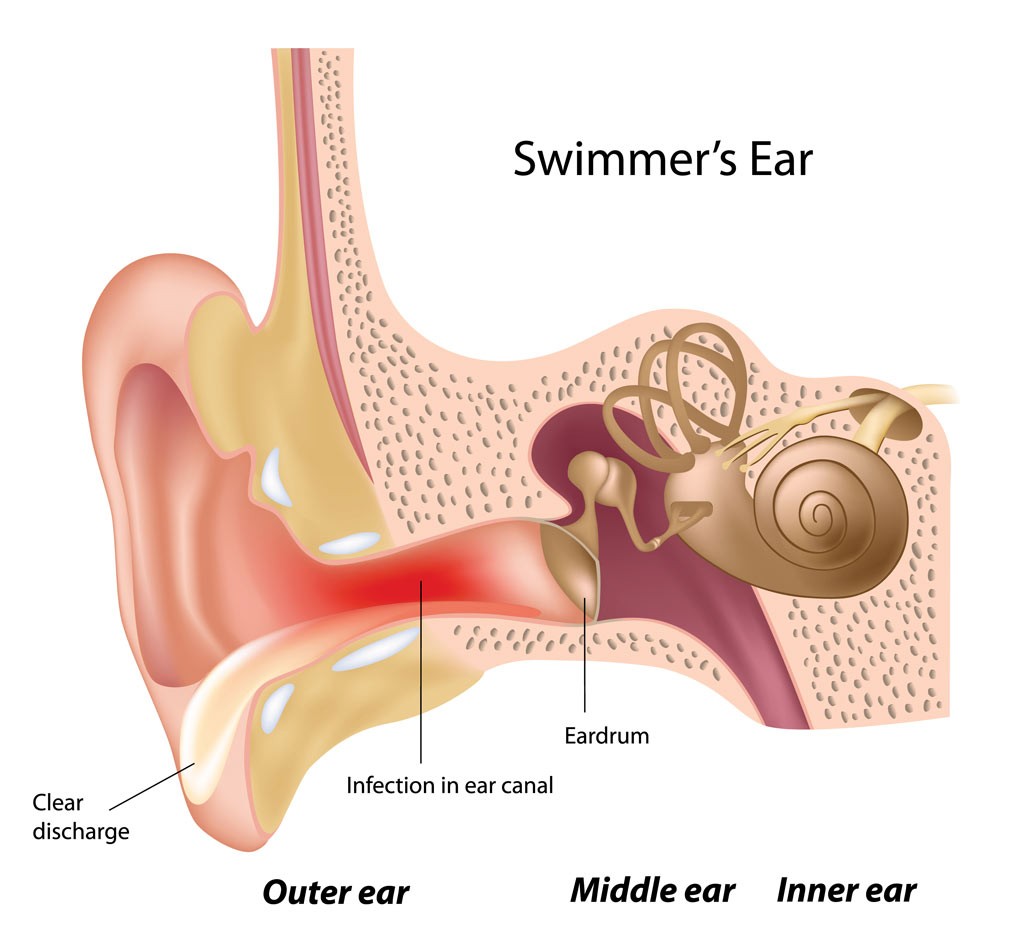
Swimmer’s ear is a condition in which the skin of the outer ear canal becomes infected, leading to inflammation and discomfort. It is typically caused by water remaining in the ear after swimming or other water-related activities, creating a moist environment ideal for bacterial or fungal growth. The condition can affect both children and adults and may manifest differently in each individual.
Symptoms of Swimmer’s Ear
The symptoms of swimmer’s ear may vary from mild to severe and can include:
- Ear pain or discomfort, which may worsen when touching or pulling the earlobe.
- Itchiness in the ear canal.
- Redness and swelling of the outer ear.
- Drainage of fluid or pus from the ear.
- Hearing impairment or a sensation of blocked ears.
- Tenderness of the ear or nearby lymph nodes.
If you experience any of these symptoms after swimming or being in contact with water, it is essential to seek medical attention promptly to prevent the infection from worsening.
Prevention of Swimmer’s Ear
Preventing swimmer’s ear is key to enjoying your aquatic activities without worry. Here are some practical tips to keep your ears safe:
- Dry your ears thoroughly: After swimming or any water exposure, gently dry your ears with a clean towel. Tilt your head to each side to help water drain out, and use a hairdryer on the lowest setting, held at arm’s length, to ensure your ears are completely dry.
- Earplugs: Wearing waterproof earplugs while swimming or engaging in water sports can be highly effective in preventing water from entering the ear canal.
- Avoid inserting foreign objects: Refrain from using cotton swabs, bobby pins, or any other objects to clean your ears, as they can push debris deeper into the ear canal, potentially leading to an infection.
- Use ear drops: Over-the-counter ear drops designed to prevent swimmer’s ear can help maintain the ear’s natural acidic environment, making it less susceptible to infections.
- Limit exposure to contaminated water: Avoid swimming in waters with high bacterial content or in areas where the water quality is questionable.
- Dry your swim gear: Ensure your swim caps, goggles, and other equipment are thoroughly dried between uses to prevent the growth of bacteria and fungi.
Treatment of Swimmer’s Ear
If you suspect you have swimmer’s ear, it is crucial to consult an ENT specialist promptly. Your doctor will examine your ear and recommend the appropriate treatment, which may include:
- Ear drops: Prescription ear drops containing antibiotics or antifungals are often prescribed to treat the infection and reduce inflammation.
- Pain relief: Over-the-counter pain relievers such as acetaminophen or ibuprofen may be recommended to alleviate discomfort.
- Avoid water exposure: While undergoing treatment, it is best to avoid swimming or submerging your head in water to prevent further irritation.
- Keep ears dry: Protect the affected ear from moisture during the healing process. Your doctor may advise using a cotton ball coated with petroleum jelly or a waterproof ear covering during showers.
- Follow your doctor’s instructions: Ensure you complete the full course of prescribed medication and follow any other advice provided by your healthcare professional.
Conclusion
Swimmer’s ear is a common and preventable condition that can put a damper on your summer fun. By following simple preventive measures, such as thoroughly drying your ears, using earplugs, and avoiding the use of foreign objects in the ear, you can greatly reduce your risk of developing this painful infection.
If you do experience symptoms of swimmer’s ear, seek medical attention promptly. Early diagnosis and appropriate treatment are essential to prevent complications and ensure a speedy recovery. Remember, a healthy and enjoyable swimming experience starts with taking care of your ears.
For more info. please visit : https://www.ahrihospital.com/