In the field of ear, nose, and throat (ENT) medicine, finding concrete solutions to complex issues requires not only expertise but also compassion and dedication. Dr. Rahul Aggarwal embodies these qualities as a leading ear, nose, and throat surgeon. Let’s explore the impact of their work and the solutions they provide to improve the lives of their patients.
A Symphony of Expertise
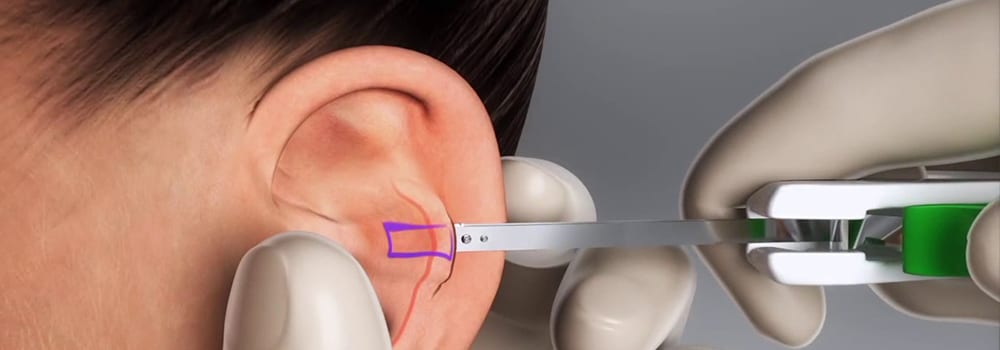
With a thorough understanding of the complex structures and functions of the ear, nose, and throat, Dr. Rahul Aggarwal holds a range of expertise in his practice. Whether addressing common ailments like sinusitis and tonsillitis or performing complex surgical procedures for hearing restoration or nasal reconstruction, Dr. Aggarwal’s precision and skill ensure optimal results for his patients.
Coherence in Compassionate Care
Beyond his technical proficiency, Dr. Rahul Aggarwal is known for his compassionate approach to patient care. He understands that seeking treatment for ENT problems can be challenging for patients, and he strives to create a supportive and empathetic environment where patients feel heard, understood, and valued. Dr. Agarwal takes the time to listen to his patients’ concerns, clearly explain their diagnosis and treatment options, and provide personalized care tailored to their individual needs.
Tuning into Innovation
As a visionary ENT surgeon, Dr. Rahul Aggarwal is constantly abreast of the latest advancements and innovations in his field. He adopts cutting-edge technologies and minimally invasive techniques to optimize surgical outcomes and minimize discomfort and recovery time for his patients. Dr. Agarwal’s commitment to being at the forefront of medical innovation ensures that his patients receive the most effective and advanced treatments available.
Echo Effect
The impact of Dr. Rahul Agarwal’s work extends far beyond the scope of his clinic. His dedication to improving the quality of life for his patients resonates throughout the community, as individuals find relief from chronic ENT conditions, regain their hearing, or breathe more easily after sinus surgery. . Dr. Aggarwal’s contribution to his field not only reduces physical discomfort but also enhances the overall well-being and quality of life of his patients.
A melody of gratitude
When we reflect on the contributions of Dr. Rahul Agarwal as an ear, nose, and throat surgeon, we are reminded of the countless individuals whose lives have been touched and changed by his care. The outpouring of gratitude from the patients who have benefited from his expertise serves as a testament to Dr. Aggarwal’s unwavering commitment to providing concrete solutions and improving the lives of those he serves.
Ultimately, Dr. Rahul Aggarwal’s dedication, compassion, and expertise make him a true expert in the field of ENT surgery. Through his concrete solutions, he continues to make a meaningful impact on the health and well-being of his patients, helping them enjoy life to the fullest.


 Introduction: Welcome to our comprehensive guide on nose care, where we delve into the intricacies of maintaining optimal nasal health. Your nose is not only essential for the sense of smell but also plays a crucial role in breathing and overall well-being. Today, we’re fortunate to have insights from Dr. Rahul Agarwal, a distinguished expert from Ahri Hospital in Gwalior, shedding light on the importance of nose care and practical tips for maintaining nasal health.
Introduction: Welcome to our comprehensive guide on nose care, where we delve into the intricacies of maintaining optimal nasal health. Your nose is not only essential for the sense of smell but also plays a crucial role in breathing and overall well-being. Today, we’re fortunate to have insights from Dr. Rahul Agarwal, a distinguished expert from Ahri Hospital in Gwalior, shedding light on the importance of nose care and practical tips for maintaining nasal health. In the bustling landscape of healthcare, certain specialists stand out for their dedication, expertise, and unwavering commitment to patient well-being. Dr. S. R. Agarwal is one such luminary in the realm of Ear, Nose, and Throat (ENT) care. With a profound understanding of the intricate mechanisms of the head and neck, Dr. Agarwal has become a beacon of hope for countless individuals seeking relief from ailments affecting these vital sensory organs.
In the bustling landscape of healthcare, certain specialists stand out for their dedication, expertise, and unwavering commitment to patient well-being. Dr. S. R. Agarwal is one such luminary in the realm of Ear, Nose, and Throat (ENT) care. With a profound understanding of the intricate mechanisms of the head and neck, Dr. Agarwal has become a beacon of hope for countless individuals seeking relief from ailments affecting these vital sensory organs.