Exploring the Connection between Ear Health and Overall Well-being By Dr. Rahul Agrawal, ENT Surgeon

Introduction:
The intricate relationship between ear health and overall well-being often goes overlooked in our daily lives. As an ENT surgeon deeply immersed in the field of otolaryngology, I am passionate about shedding light on the profound impact that ear health has on our holistic health. In this article, we will explore the multifaceted connection between the ears and overall well-being.
The Ear-Body Connection:
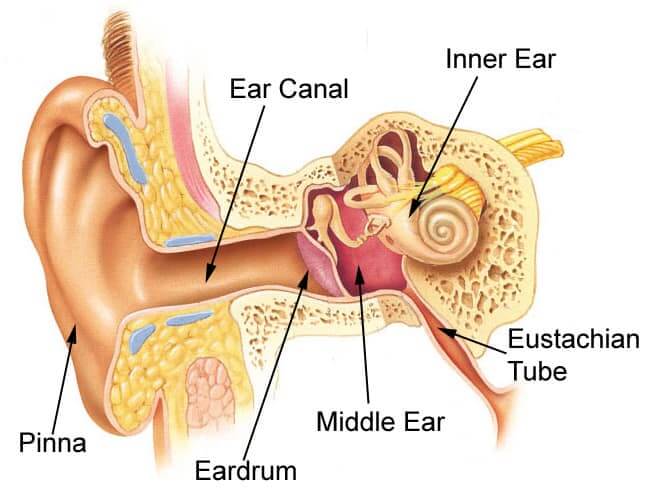
Our ears are not isolated entities; they are integral parts of our sensory system and are intricately connected to our overall health. The auditory system not only enables us to hear but also plays a vital role in maintaining balance and spatial orientation. Additionally, the ear is linked to the nervous system, influencing various bodily functions.
Hearing Health and Cognitive Function:
Research has established a strong correlation between hearing health and cognitive function. Untreated hearing loss has been linked to an increased risk of cognitive decline, dementia, and Alzheimer’s disease. As an ENT surgeon, I often emphasize the importance of regular hearing check-ups, especially for older individuals, to address hearing issues promptly and potentially mitigate cognitive risks.
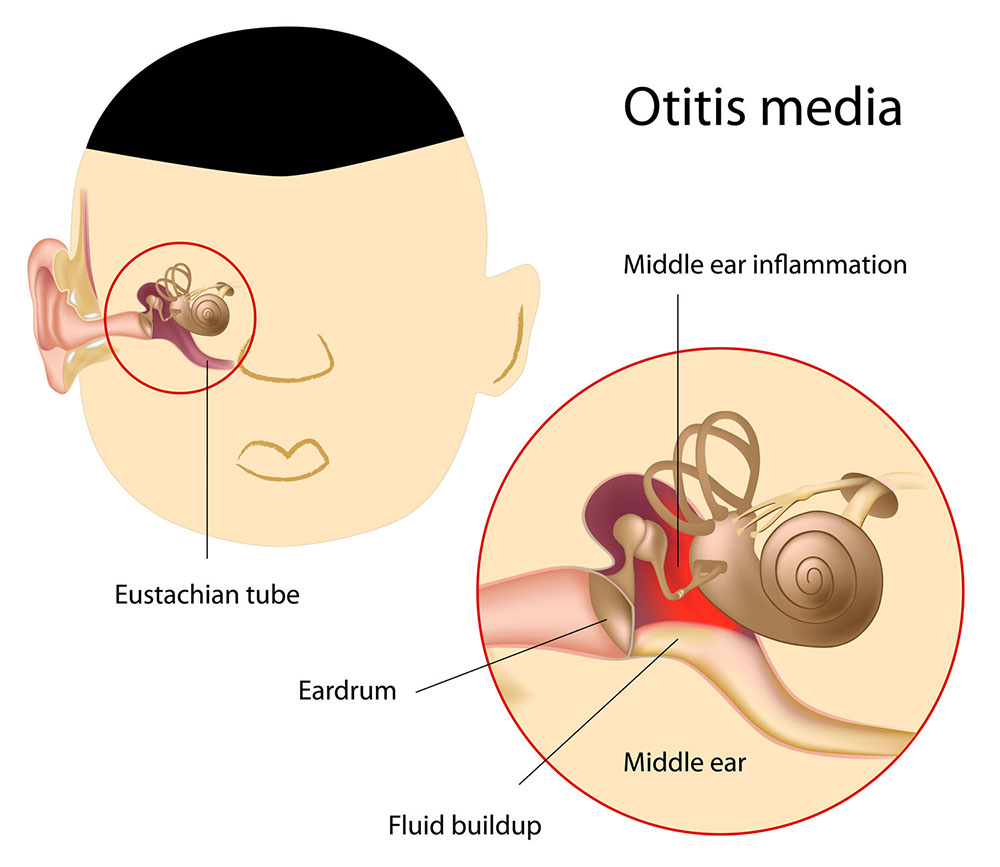
The Impact of Ear Infections on General Health:
Ear infections, common in both children and adults, can have implications beyond temporary hearing loss and discomfort. Chronic ear infections, if left untreated, may lead to complications such as balance problems, facial nerve paralysis, and even systemic infections. Timely intervention is crucial to prevent these issues and safeguard overall health.
Ear Health and Emotional Well-being:
The emotional toll of hearing impairment should not be underestimated. Individuals experiencing hearing loss may face challenges in communication, leading to feelings of isolation and frustration. Addressing hearing issues through appropriate interventions, such as hearing aids or surgical procedures, can significantly enhance emotional well-being and quality of life.
The Role of Ear Health in Preventing Falls:
The inner ear plays a pivotal role in maintaining balance and preventing falls. Disorders affecting the vestibular system, such as Meniere’s disease or benign paroxysmal positional vertigo (BPPV), can result in dizziness and an increased risk of falls. By prioritizing ear health, especially in older individuals, we can contribute to fall prevention and overall safety.
Noise-Induced Hearing Loss and Lifestyle Choices:
In our modern, noisy environments, protecting our ears from excessive noise is crucial. Noise-induced hearing loss, often a result of prolonged exposure to loud environments, can impact our ability to perceive and respond to auditory stimuli. Incorporating ear protection measures, such as earplugs or noise-canceling headphones, is a proactive step toward preserving both hearing health and overall well-being.
Preventive Measures and Healthy Habits:
Regular ear check-ups, prompt treatment of ear infections, and adopting lifestyle habits that promote ear health are essential components of preventive care. As an ENT surgeon, I encourage individuals to be mindful of their ear health, just as they would be of any other aspect of their well-being.
Conclusion:
The intricate connection between ear health and overall well-being highlights the importance of considering our auditory system as a vital component of our holistic health. By understanding and prioritizing ear health, we can make informed choices that positively impact not only our ability to hear but also our cognitive function, emotional well-being, and overall quality of life. As we embark on a journey toward comprehensive health care, let us not overlook the significance of preserving and nurturing our precious sense of hearing.
For more info. please visit : https://www.ahrihospital.com/